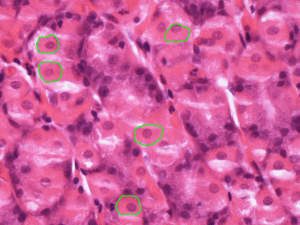
Have you ever wondered what stomach cells would do if given another job? Probably not, but a group of scientists from Weill Cornell Medicine in the USA did. And there was an answer, too.
The researchers turned stomach cells into tissues capable of releasing insulin in response to rising blood sugar levels. The discovery, published in Nature Cell Biology (I link it to you here) can be a very important step forward in the management of conditions such as type 1 diabetes.
Hard work
Usually, the job of releasing insulin in response to rising blood sugar levels falls to the beta cells of the pancreas. In diabetics, however, these tissues can become damaged or die, compromising their ability to transport glucose into cells to transform it into energy.
This is why GINS cells (acronym that stands for Gastric Insulin-Secreting) were conceived, wanted, sought, obtained, i.e. the gastric cells that secrete insulin. Although they are not beta cells, they can mimic their function. We are chock full of stem cells, capable of transforming into various types of cells and proliferating rapidly.
The goal is to ensure that diabetics can have their intestinal stem cells transformed into GINS cells, limiting the risk of rejection.
From the stomach with fury

Secondo Joe Zhou, an associate professor of regenerative medicine at Weill Cornell Medicine in New York, it's not such a surprising discovery that gastric stem cells can be transformed into beta cells. After all, stomach cells make their own hormone cells, and in the embryonic stage, stomach and pancreas cells are adjacent.
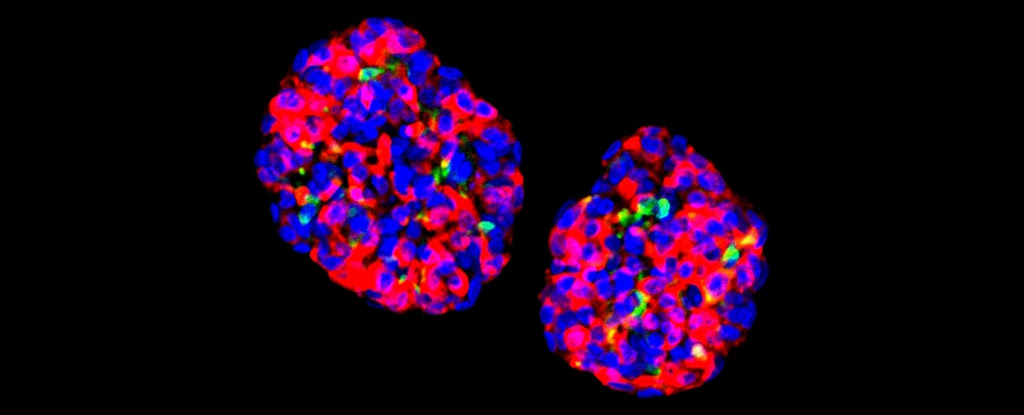
The research team activated three specific proteins in the cells that control gene expression, in a particular order, to trigger the transformation into GINS cells. This reprogramming process proved to be very efficient: the cells, grown in small groups known as organoids, showed glucose sensitivity and produced long-lasting effects on diabetes in mice.
Creating GINS cells isn't a particularly complicated process, say the researchers. It only takes a few days, and these new organoids can last for many months after being transplanted, according to their tests.
Next steps
The research is still in its infancy, but it could allow the body to manage insulin levels more naturally. There are several differences between human and mouse stomach tissue that need to be addressed in future studies, and GINS cells need to be made less vulnerable to attack by the immune system.
Despite this, the first signs are enormously promising. “This study gives us a solid foundation to develop a treatment, based on the patient's own cells, for type 1 diabetes and severe type 2 diabetes,” says Zhou.