In a pilot study, the implant restored sight to 20 people with diseased corneas: most of these were blind before receiving it. The promising results bring hope to those suffering from blindness and corneal low vision. They can bring a bioengineered implant as an alternative to transplanting donated human corneas, which are in short supply in countries where the need is greatest.
An implacable enemy
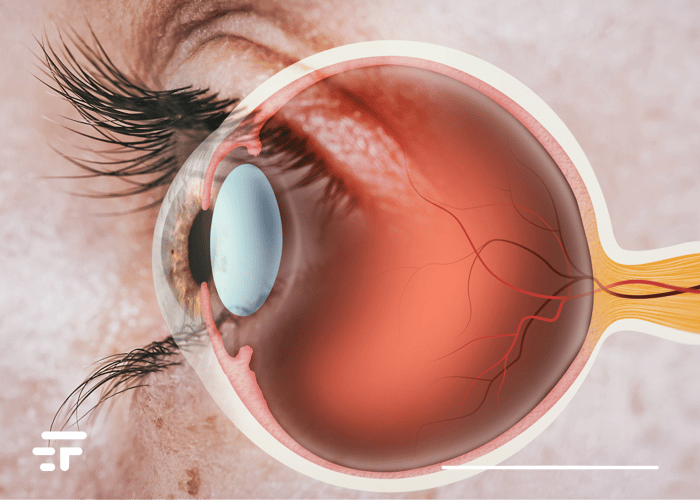
An estimated 12,7 million people worldwide are blind due to damage or disease to the cornea, the outermost transparent layer of the eye.
The only way to regain sight is to receive a transplanted cornea from a human donor. But only one in 70 patients receives a cornea transplant. Furthermore, the majority of those who need a corneal transplant live in low- and middle-income countries, where access to treatments is very limited.
The results of this new and recent study are very important and bode well for the future.

The bioengineered cornea?
The cornea is mainly made up of the protein collagen. To create an alternative to the human cornea, researchers used collagen molecules derived from pig skin, highly purified and produced under rigorous conditions for human use.
The pig skin used is a by-product of the food industry, easy to find and economically advantageous.
In the process of building the implant, the researchers stabilized the loose collagen molecules. The process formed a strong, transparent material that could withstand handling and implantation in the eye. While donated corneas must be used within two weeks, bioengineered ones can be stored for up to two years before use.
“The safety and effectiveness of bioengineered implants have been the focus of our work,” he says Mehrdad Rafat, researcher and entrepreneur who designed and developed the systems. Rafat is an adjunct associate professor (senior lecturer) in the Department of Biomedical Engineering at LiU and the founder and CEO of the company LinkoCare Life Sciences AB, which produces the bioengineered cornea used in the study (that I link to you here).

Cornea transplant: the new solution
Researchers have also developed a new, minimally invasive method to treat keratoconus disease, in which the cornea becomes so thin that it leads to blindness.
Today, the cornea of a patient with advanced stage keratoconus is surgically removed and replaced with a donated cornea, which is sewn into place with surgical sutures. This type of surgery is invasive and is performed only in larger university hospitals.
“A less invasive method could be used in more hospitals, thus helping more people. With our method, the surgeon does not need to remove the patient's tissue. Instead, a small incision is made, through which the implant is inserted into the existing cornea,” he says Neil Lagali, leading the research team that developed this surgical method.
With this new surgical method no stitches are necessary. The incision in the cornea can be made with high precision thanks to an advanced laser, but also, when necessary, by hand with simple surgical instruments.
The method was first tested on pigs and proved to be simpler and potentially safer than a conventional cornea transplant.
It works?
The surgical method and implants have been used by surgeons in Iran and India, two countries where many people suffer from corneal blindness and low vision, but where there is a significant lack of donated corneas and treatment options.
Twenty people who were blind or on the verge of losing their sight due to advanced keratoconus participated in the pilot clinical study and received the biomaterial implant. The surgeries were complication-free, the tissue healed quickly, and an eight-week treatment with immunosuppressive eye drops was sufficient to prevent rejection of the implant.
With conventional corneal transplants, the medications must be taken for several years. Patients were followed up for two years, during which time no complications were found.
The main aim of the pilot clinical study was to verify the safety of the implant. However, researchers were surprised by what happened with the implant. The thickness and curvature of the cornea returned to normal. At the group level, participants' vision improved as much as it would have improved after a cornea transplant with donated tissue. Before the intervention, 14 of the 20 participants were blind. After two years, none of them were blind anymore.
Three of the Indian participants who had been blind before the study had perfect vision (20/20) after the operation.
Then? Will treating the cornea no longer be a problem?
Caution! Before the implant can be used in a healthcare setting, a larger clinical study is needed followed by approval from regulatory authorities.
The researchers also intend to study whether the technology can be used to treat other eye conditions and whether the implant can be tailored to the individual to achieve even greater effectiveness.
“The results demonstrate that it is possible to develop a biomaterial that meets all the criteria for use as a human implant, which can be mass-produced and stored for up to two years, thus reaching even more people with vision problems. This allows us to circumvent the problem of shortage of donated corneal tissue and access other treatments for eye diseases,” says Lagali.
“We have made significant efforts to ensure that our invention is widely available and accessible to everyone, not just the wealthy. That is why this technology can be used in all parts of the world,” Rafat finally declared.
The conditions are very promising, both in medical and ethical terms; all that remains is to wait and observe the developments!


