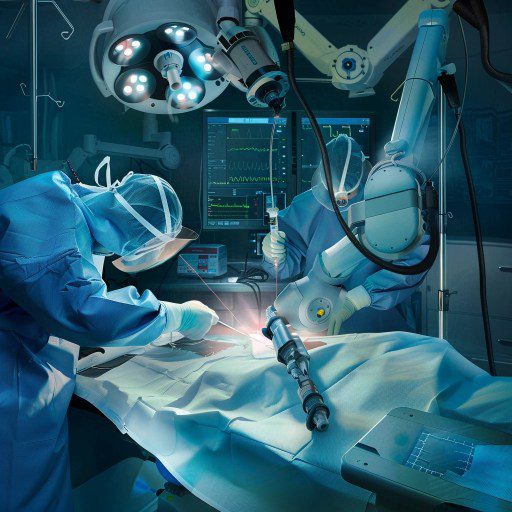
A video of a surgical robot sewing together a grape that went viral nearly 10 years ago has put a spotlight on a rapidly evolving technology: robotic surgery. Since then, this sector has experienced massive growth in terms of technological capabilities, investments and the number of robot surgeons deployed worldwide.
Behind the promises of less invasive interventions and faster recoveries, however, there are still doubts about the actual effectiveness of some expensive machines and their acceptance by patients and surgeons in the flesh.
Robot surgeons enter the operating room
Traditional surgery is a highly invasive procedure. To perform an operation, the surgeon must make a large incision, large enough to allow his hands and instruments access to the affected body part. After surgery, the patient then faces a recovery that can be long, painful and uncomfortable.
To overcome these problems, surgeons have introduced laparoscopic surgery, which requires only small incisions to insert thin tubes with specialized instruments and a camera. An important technique, which reduced recovery times and post-operative pain compared to traditional surgery.

Robotic surgery represents a further step forward. As in laparoscopy it requires only small incisions, but the key difference is in the control of the instruments: in robotic surgery, the surgeon maneuvers them via a robot, using specialized commands that translate his movements into precise actions within the patient's body.
A growing market
The first surgical robot to gain FDA approval was the System Da Vinci, developed by Intuitive Surgical, in 2000. Since then, Intuitive has become an industry leader, with over 7500 Da Vinci robots in use worldwide. Every 17 seconds, somewhere in the world, a surgeon begins an operation using one of these robots.
Other market players include Medtronic with the Hugo robot, Johnson and Johnson with Ottava, Stryker with Mako, CMR with versius and Vicarious Surgical. Even Google, through its life sciences company Verily, partnered with Johnson & Johnson to create a surgical robot in 2015.
Secondo a relationship by Bain & Company, the robotic surgery market was worth between $3 billion and $3,5 billion at the start of 2023, up from $800 million in 2015. Another report estimates the market value will reach $11,76 billion dollars by 2029. The image that emerges is that of a growing sector with a multi-billion dollar value.
The dream of remote surgery
Robot surgeons open up the possibility of performing remote surgeries. The first truly complete remote surgery was conducted on September 7, 2001 across the Atlantic Ocean, with a surgeon in France operating on a patient in New York at a distance of 6.230 km. Remote surgeries are possible, but the biggest challenge preventing them from becoming common is network speed. This type of procedure requires ultra-fast networks with as little delay as possible. As networks become faster and more reliable, the prospect of remote surgeries becoming common practice grows closer.
Such procedures could allow world-class specialists to perform surgeries anywhere in the world, opening access to the best surgeons to more patients, regardless of where they are located. The military could also be interested: the best surgeons could save soldiers' lives while remaining safe, away from active combat zones.
Remote surgeries also open up the possibility of performing operations in space. A surgeon can remain on Earth while a robot translates his movements onto a patient in Earth orbit. While this vision is still far in the future, NASA is exploring the concept of robot surgeons in space with MIRA, a small surgeon robot developed by researchers at the University of Nebraska-Lincoln. The next step for MIRA is to be launched to the International Space Station in 2024 to test its robustness and performance in weightlessness.
Towards autonomous robot surgeons?
Are we close to having fully autonomous robot surgeons? In short, no. None of the currently available surgeon robots are fully autonomous. Robots like Da Vinci are directly controlled by human surgeons all the time. Some medical robots, such as the CyberKnife, a robotic system designed for radiotherapy, are to some extent autonomous, but still require human supervision.
Creating a fully autonomous surgeon robot is the industry's holy grail, but there's no indication that such robots will arrive anytime soon. The ability to autonomously perform a complex task represents a huge challenge for AI researchers and robotics engineers. Simpler aspects of surgical procedures, such as wound closure, are more likely to be automated first, leaving the surgeon to focus on the main procedure.
However, there are research projects that push towards the vision of a completely autonomous surgeon robot. An example is STAR, a surgical robot developed at Johns Hopkins University (JHU), which successfully performed near-autonomous surgery on a pig. Quasi, because STAR needed a little help from a human. As the JHU team said, a fully autonomous STAR is probably decades away, but they will continue to work in the hope that in about five years the technology will advance to the point where a first clinical test in a human is possible. Who raises their hand first? Congratulations.
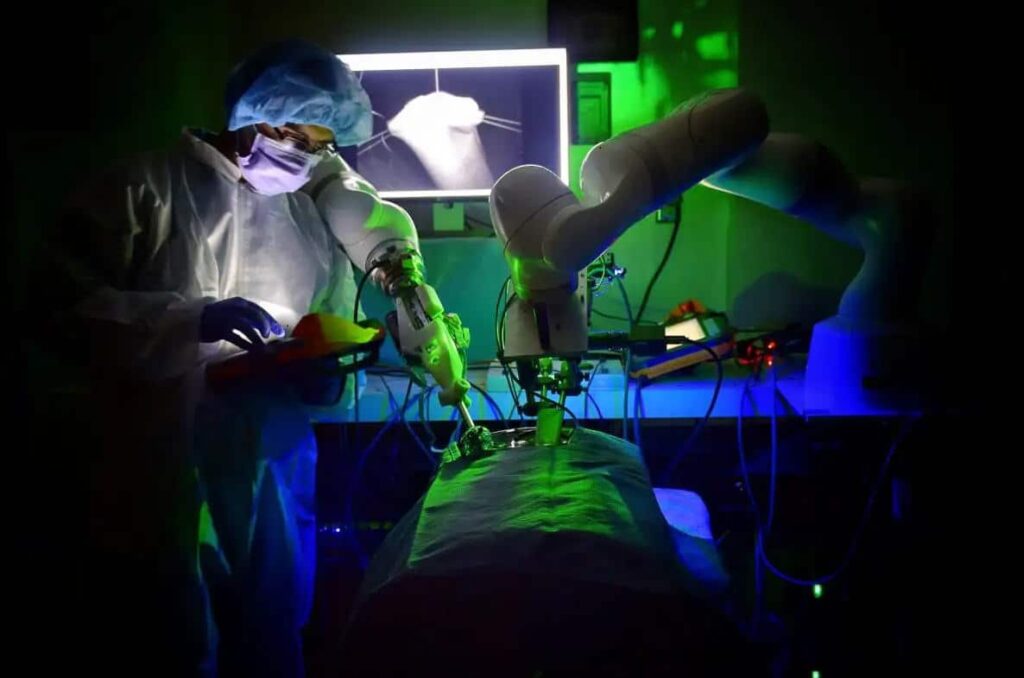
Robot surgeons, advantages and challenges
Surgical robots bring and will bring many good things, beyond smaller incisions, faster recovery and less post-operative pain. Human surgeons also benefit from this: the operations are less tiring and the instruments more precise and easier to handle. Thanks to better visualization tools, real professionals can access much more information during the operation.
However, the adoption of these robots also presents obstacles. First, the cost: Buying and maintaining a surgical robot can cost millions of euros, putting them out of reach for many hospitals. Furthermore, despite the potential benefits, patients still appear to prefer human surgeons to robots. Several studies have shown that, given the choice, most people would opt for traditional laparoscopic surgery. An understandable distrust, which only time and examples will be able to address.
More research is needed
We currently lack enough data to determine how much robotic surgery really makes a difference. The Royal College of Surgeons of England recognizes the potential benefits of this technology, but says there is a lack of good quality data to establish how much robot surgeons actually improve accuracy, efficiency and patient safety.
Where comparisons have been made between robotic and laparoscopic surgery, there appears to be little or no difference, with the only clear discrepancy being that robotic surgeries take longer. Further studies are needed to evaluate the real impact of robot surgeons and whether they are really worth the investment.
In any case, it is clear that the future of surgery will be increasingly robotic. The adoption and public perception of this technology mirrors the path followed by laparoscopy: it took years for the latter to be considered safe and widely accepted by patients and surgeons. Robotic surgery is currently going through this phase.
It is likely that we will see more and more robot surgeons in the operating room, ready to take up the scalpel... or whatever instrument the future holds.