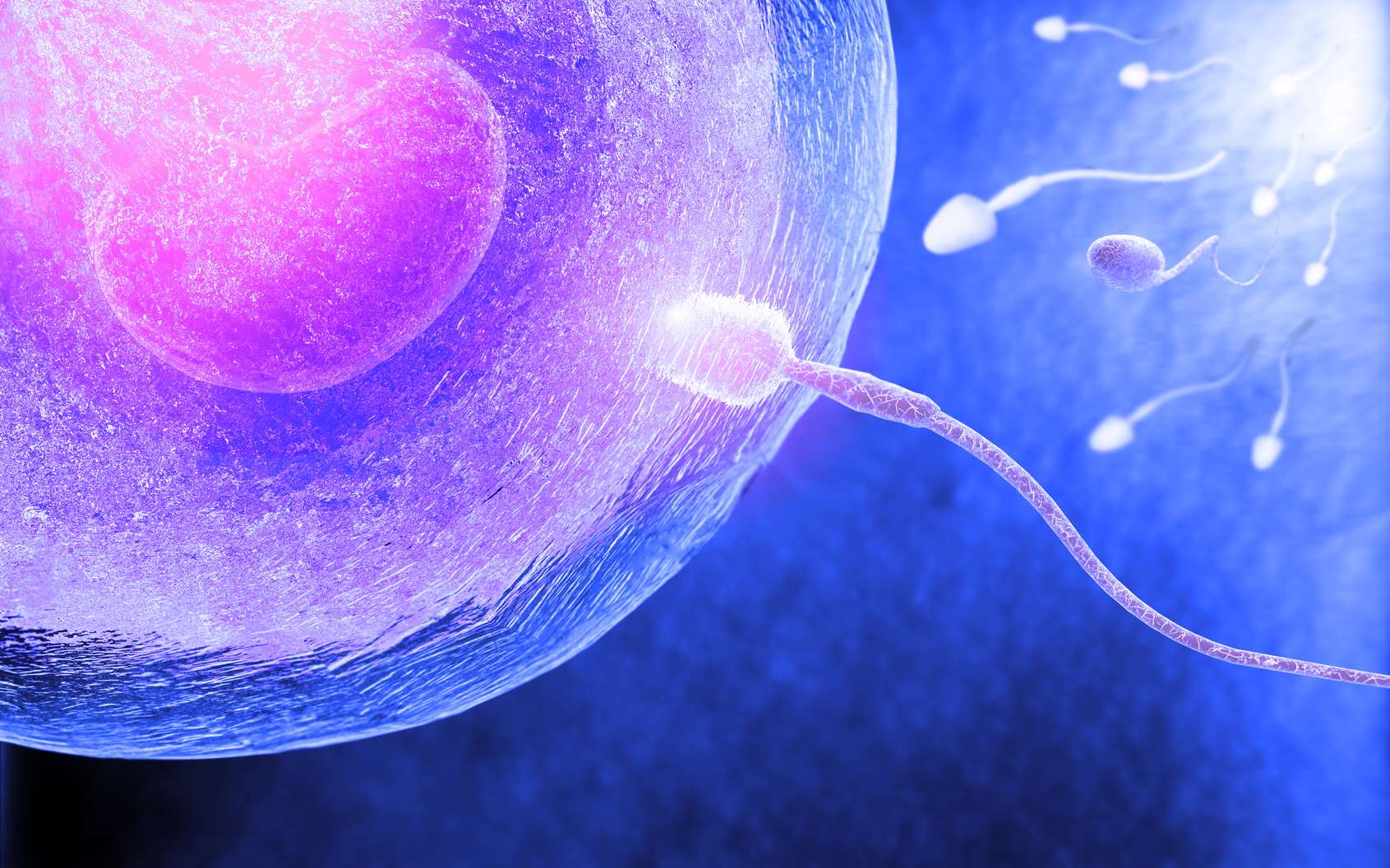
For many women, preventing pregnancy means using contraceptives that can have serious, potentially serious, side effects. A research team works on a different type of contraceptive based on engineered antibodies. Antibodies that bind to spermatozoa and "capture" them to prevent them from entering the vaginal mucus.
I know it sounds strange (to me at least), but the specially designed antibodies have proved to be an amazing solution. Powerful, stable and over 99% effective (in sheep tests) in stopping sperm movement.
An anti pregnancy "vaccine"?
“Although human testing is needed, these antibodies may offer women an alternative to hormonal contraception,” says the immunologist Bhawana Shrestha, first author of the published article, describing how antibodies can slow down avoiding unwanted pregnancy.
The sperm must swim through the mucus and up the female upper reproductive tract to reach and fertilize the egg. Typically only about 1% of ejaculated sperm enters the cervix. But just one sperm is enough to start a pregnancy.
From the article of the research team
Current anti-pregnancy methods need to be improved
Among the contraceptive methods More reliable, many are hormonal contraceptives that work by providing constant doses of sex hormones to prevent the release of eggs from the ovaries. The contraceptive pill, implant and vaginal ring are some examples that are very effective in preventing pregnancy if used correctly.
Unfortunately, some users of hormonal contraceptives experience serious side effects. The spectrum is broad: from weight gain and low libido, from migraines to mood changes. Even depression. There are other risks too, such as increased chances of blood clots and breast cancer.
It doesn't surprise me, therefore, why some women want non-hormonal options to prevent pregnancy.

The alternative
There is a clear need for large-scale clinical trials of new and existing forms of birth control. Yet, despite this, little is invested in this direction. Not only that: apart from the economic question, the approaches are always the same. Or rather, they were until yesterday.
The study conducted by Shrestha at the University of North Carolina takes a totally new path. The team focuses on antibodies, the Y-shaped molecules that immune cells produce to neutralize infections or foreign particles.
Some women, absolutely healthy but with a condition called immune infertility, they produce anti-sperm antibodies in their reproductive tract that block any pregnancy. Using these antibodies as a scaffold, the researchers designed a series of antibodies engineered to improve their capabilities.
Laboratory tests
In the first stage, the antibodies were subjected to a “sperm escape test”. The researchers quantified how many sperm cells could escape antibody traps in a plastic tube filled with vaginal mucus.
Compared to the original anti-sperm antibodies, the modified antibodies were at least 8 times better in pooling spermatozoa, preventing pregnancy.
The next test consisted of injecting antibody solutions, followed by (human) sperm samples into the vaginas of several sheep. After just two minutes, the antibody treatment had reduced the number of motile sperm in the recovered fluid samples by at least 97%.
How to apply the method to humans?
This could be done in several ways: a kind of film that dissolves quickly or “intravaginal rings” that allow a constant release of antibodies, just like a traditional contraceptive, but without the presence of hormones.
We are actively pursuing the development of an intravaginal ring capable of releasing these antibodies and anticipating the insights that will emerge in the years to come.
From the team article
There is still a long way to go for the development of this anti-pregnancy solution in humans. Rigorous clinical studies on humans are obviously needed.
If the method proves effective in preventing pregnancy in further trials, however, this system will have several health benefits for patients. Rather than altering the physiological mechanisms underlying fertility, in fact, topical immunocontraception should allow a rapid return to fertility.
Quite a difference from the months of delay experienced by some women even after stopping use of long-acting hormonal contraceptives.
The research was published in Science Translational Medicine.