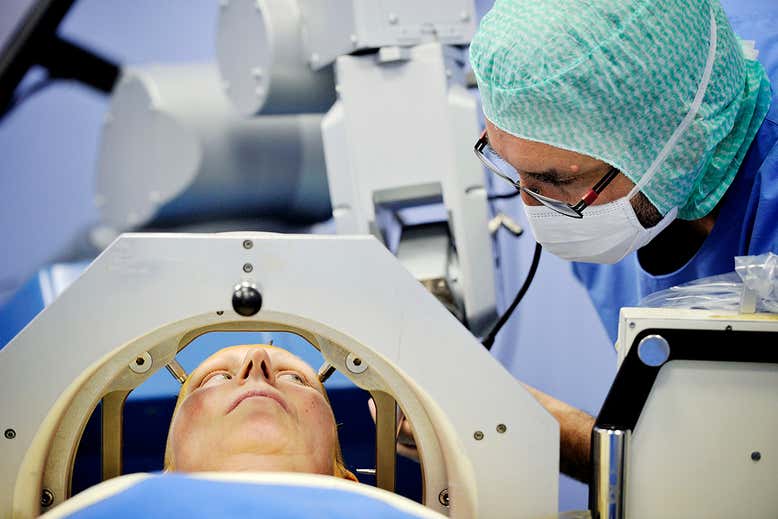
Several Parkinson's disease patients are receiving brain implants that can automatically detect and reduce the activity of harmful nerve cells, to see whether the technique will reduce movement difficulties. The device is a step forward compared to a conventional brain implant because it is designed to also reduce the side effects of its own “installation”.
Parkinson's disease causes worsening of tremors and difficulty moving, especially when in the initial phase of movement. Medications can help, but as symptoms progress some people have a more drastic treatment called deep brain stimulation (DBS).
Deep brain stimulation in patients with Parkinson's disease
This treatment works by placing electrodes in the skull that deliver a current to dampen activity in groups of nerve cells in the center of the brain. However, there are side effects, such as speech difficulties and jerky movements. It may be possible to minimize these side effects by providing stimulation only when needed (known as “reactive stimulation”). The activity of nerve cells can be recorded by the same “wire” that supplies the current.
A similar type of brain implant is already used in some people with severe epilepsy that doesn't respond to drugs or surgery, to reduce the excessive activity of nerve cells that causes seizures. But in people with Parkinson's it is less clear what type of brain activity causes different symptoms and side effects.
Brainwave targets
The area most suspected is that of "clusters of nerve cells" affected in some way by brain implants in patients with Parkinson's disease. In most people, these centers sometimes activate in patterns called “beta waves” to signal to continue the current behavior, whatever it may be. “It promotes the status quo,” he says Peter Brown at Oxford University. In Parkinson's there is an excess of beta waves, and this may explain why people with the condition sometimes move more slowly than they want and have difficulty initiating new movements.
Brown and his colleagues are looking to stimulate nerve cell clusters only when beta waves are detected.
The team tried the technique in 13 people with Parkinson's who had a particular problem moving too slowly while they were having surgery under local anesthesia to replace the battery in their existing DBS implant. Brown's team found that the reactive stimulation caused fewer speech disorders compared to conventional constant stimulation and was equally effective in fighting slow movements.
“Problems with speech are currently one of the most problematic side effects of standard DBS”, he claims David Dexter at Parkinson's charity in the UK. “This can have a huge impact on your quality of life.”
And for the tremors?
Tim Denison at the University of Oxford is trying to develop another type of implant that targets the other main side effect of DBS, jerky involuntary movements. By introducing a second connector to the surface of the brain, his team discovered that these movements are accompanied by another type of brain wave (gamma waves) in an area called motor cortex.
A team led by Aysegul Gunduz at the University of Florida is conducting a test on 20 people with Parkinson's disease to reduce some types of tremors with this type of system.
Reference : bioRxiv, DOI: 10.1101/749903