Australian researchers have developed a technique to awaken pancreatic stem cells and produce insulin: it could be a new approach to treating type 1 diabetes.
They did this using a drug already approved by the FDA, but not yet for the treatment of diabetes. Although the research is still in the early stages, this method could lead to future therapies in which newborn insulin-producing cells (beta-cells) will be used to replace those destroyed in type 1 diabetics. The results have been presented in a new study. published in the journal Signal Transduction and Targeted Therapy (I link it here).
“It is an important step forward towards the development of new therapies,” says senior author Professor Assam El Osta, epigeneticist and leader of the research group at Monash University, Australia.
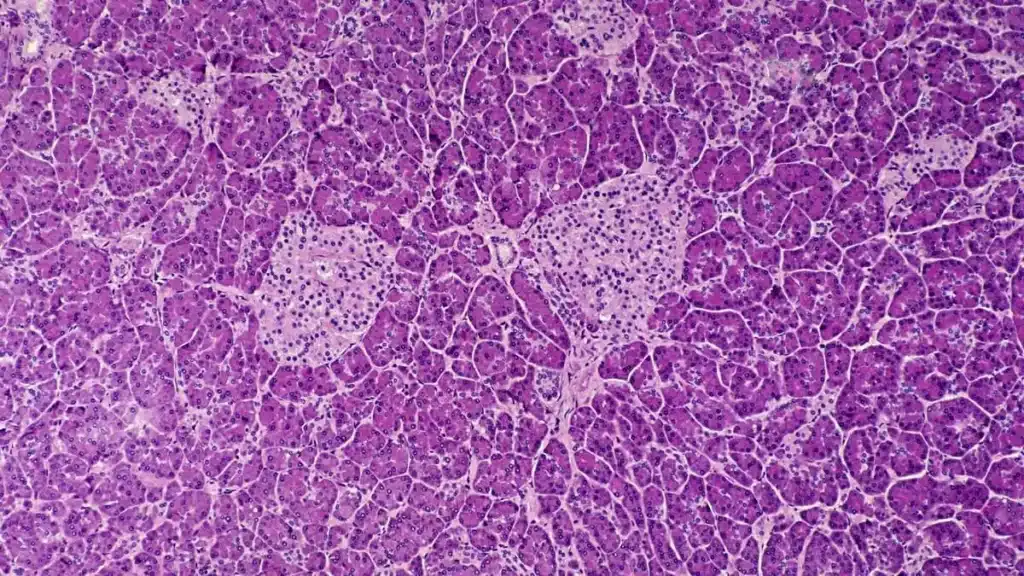
Reprogram the stem cells of the pancreas
Type 1 diabetes is an autoimmune disease in which the insulin-producing beta cells in the pancreas are selectively destroyed.
“Patients rely on daily insulin injections to compensate for the pancreas' failure to produce it,” explains El-Osta. “Today the only alternative therapy requires pancreatic islet transplantation, but it relies on organ donors. This is why it has a very limited diffusion."
Pancreatic progenitor cells are stem cells with the ability to differentiate into various cells of the pancreas, including beta cells. To reprogram these cells to make insulin (and then feed them back into the pancreas), the team collected it from a donor with type 1 diabetes and two non-diabetic donors.
These cells were then treated with an ingredient called GSK126. The result? The researchers restored insulin gene expression in these cells.
Implications for future diabetes care
There are currently some limitations to consider. The first: the study still involves too few subjects to be sure that it will be possible to generalize. Ditto for the effects: will they be transient or long-term?
More work will be needed to define the properties of these cells, and to establish the protocols necessary to isolate and expand them. A therapy is still over the horizon at the moment.
However, the study is indeed a very important step along the way to devising a lasting treatment that could (this would be the breakthrough) be applicable to all types of diabetes.



